
Table of contents
What is Prior Authorization in Healthcare?
How AI-Native Prior Authorization Agents Deliver Faster Decisions
How MoolAI's Architecture Supports Faster, More Accurate Prior Authorization
Outcomes from MoolAI's Pilot
What to Expect When Deploying MoolAI's Prior Authorization Agent
Somewhere in the United States, a patient is waiting for cancer treatment. Their oncologist has prescribed it. The pharmacy is ready. The appointment is scheduled. Yet care is paused by a single missing piece of paperwork: a prior authorization waiting in a payer's queue.
According to the American Medical Association, the average prior authorization turnaround is nearly two weeks. Each year, millions of authorizations are denied, often because of insufficient information, missing documentation, or rework caused by manual errors.
Physicians and their staff spend more than thirteen hours every week processing these requirements. More than eight in ten physicians report that prior authorization delays have caused patients to postpone, or even abandon, their recommended treatment.
This is not just an administrative concern. It is a healthcare problem with real consequences for patients. Every delayed approval can mean delayed relief, deteriorating health, and in some cases, a treatment plan abandoned altogether.
In this article, we look at how prior authorization actually works, why it takes so long, and how MoolAI's AI-native Prior Authorization Agent gets approvals through in days instead of weeks.
What is Prior Authorization in Healthcare?
Prior authorization is a verification process used by health insurance companies to determine whether a diagnostic test, prescribed treatment, procedure, or medication qualifies for coverage before it is delivered. When a healthcare provider recommends a specific treatment, they must submit clinical documentation to the insurer to demonstrate medical necessity and alignment with the patient's coverage.
The payer reviews the request against established guidelines and either approves it, denies it, or requests additional information. Only after approval can the provider be sure the treatment will be reimbursed under the patient's plan.
Because of the multiple verification steps and the volume of documentation required, the process can take up to two weeks. That delay creates anxiety for patients, fatigue for healthcare staff, and real financial pressure on the practice.

An efficient, accurate, and automated prior authorization system is no longer a nice-to-have. It is essential.
How AI-Native Prior Authorization Agents Deliver Faster Decisions
Traditional prior authorization workflows are slow because they rely on disconnected systems, manual data entry, and repetitive verification tasks done by humans.
AI-native prior authorization automates the entire workflow, from data extraction and validation through submission and status tracking. Instead of relying on a single monolithic model, AI-native systems deploy multiple specialized agents working in parallel.
The result is faster approvals, higher first-pass acceptance rates, fewer manual errors, and a meaningful reduction in administrative burden. Most importantly, patients gain quicker access to the care they need.
How MoolAI's Architecture Supports Faster, More Accurate Prior Authorization
MoolAI built its Prior Authorization Agent on a multi-agent orchestration architecture, where each agent performs a specialized task while working seamlessly with the others.
An RPA agent extracts patient data directly from the EMR, including legacy systems without API connectivity.
A data agent standardizes and enriches the information.
Three verification agents simultaneously validate patient eligibility, provider NPI, and CPT code requirements.
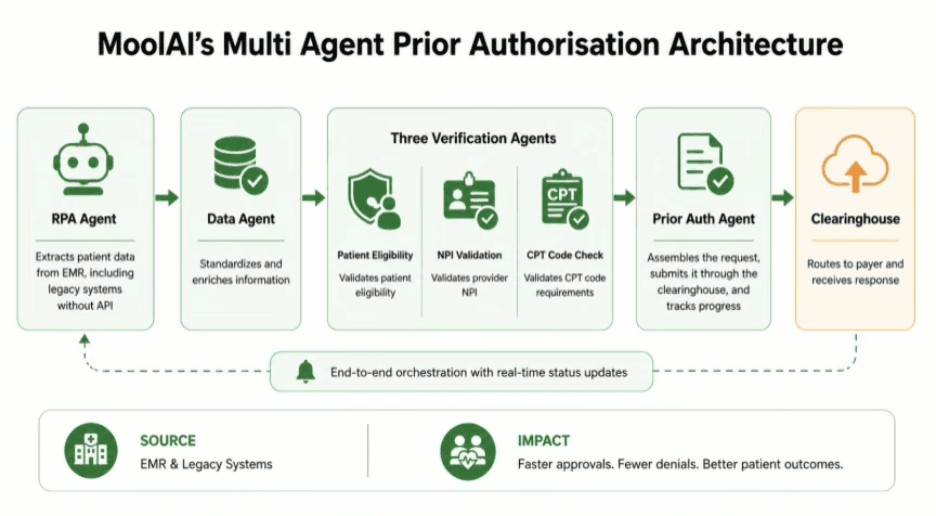
Finally, the Prior Authorization Agent assembles the request, submits it through the clearinghouse, and tracks its progress.
This architecture removes manual handoffs, reduces errors, and accelerates approvals.
Outcomes from MoolAI's Pilot
In a leading oncology network processing approximately 1,600 prior authorizations daily, approval times dropped from two weeks to just one or two days. First-pass approval rates improved significantly.
Security and compliance are foundational. The agents operate entirely within the customer's cloud environment. Patient data never leaves their infrastructure. Personally identifiable information is masked before any model interaction, and every decision is logged for transparency, governance, and HIPAA alignment.
What to Expect When Deploying MoolAI's Prior Authorization Agent
But the metrics tell a larger story. They represent patients accessing critical treatments sooner, providers spending less time on paperwork, and care teams focusing on the decisions that truly need human judgment.
That is the work. Not faster paperwork. Faster care.
Try MoolAI today.
Build agents. Trust their outputs. Scale confidently.
Moolai ensures every AI agent is reliable, governed, and ready for enterprise deployment.
Book your Demo
MoolAI
MoolAI is an AgaaS ( Agent as a Service) platform for B2B SaaS taking enterprises from AI pilots to production in one click
All copyrights are reserved MoolAI Inc